

The Problem
-
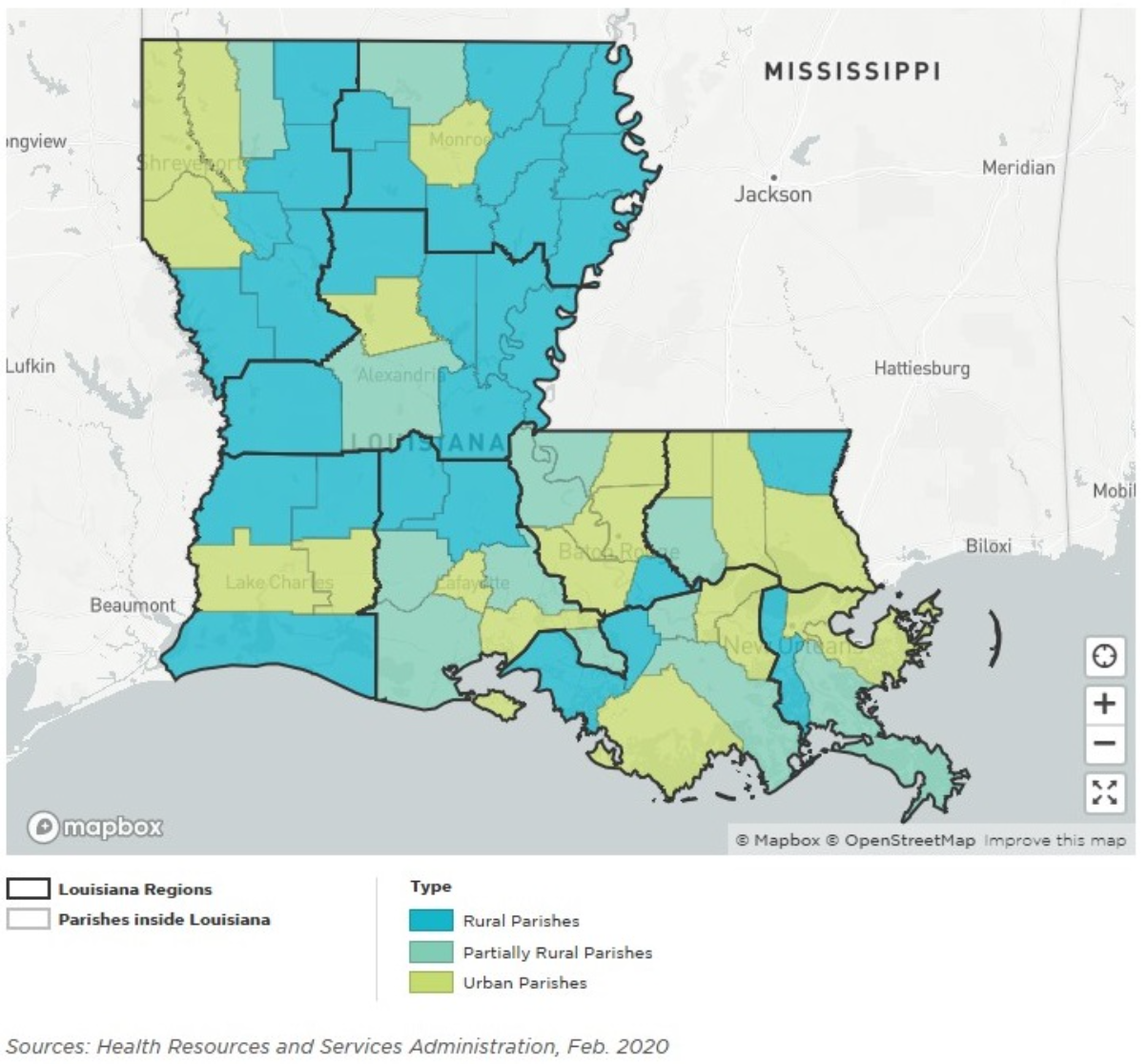
Over 1.2 million Louisianans (about 26-27% of the population) live in rural areas, facing persistent poor access to primary and specialty care, including radiology/imaging services, which contributes to worse cancer outcomes (Louisiana Comprehensive Cancer Control Plan 2022-2027; Feeding Louisiana, 2020).
-
Rural Louisiana parishes show a wide gap in cancer mortality rates compared to urban areas, with rural residents experiencing higher overall cancer death rates due to limited access to screening, diagnostics, and follow-up (Louisiana Comprehensive Cancer Control Plan 2022-2027).
Currently, 60–80% of incidental findings discovered in rural ERs are lost to follow-up. This "diagnostic gap" represents a massive clinical liability and a multimillion-dollar revenue leak for rural hospitals. The 50% Rule: Industry data confirms that 50% of all recommended radiology follow-ups are never completed. In rural ER settings, this failure rate spikes as high as 78% due to communication gaps between the ER and primary care (JACR 2022).
Only 33% of patients with incidental lung nodules received any follow-up care within the first year. Even for "high-risk" nodules, the failure rate was over 60% (Blagev et al, CHEST 2014).
-
Follow-up for imaging findings shows low completion rates overall (~17-30% in some ED settings), with rural challenges amplified by distance, limited specialists, and travel—exacerbating missed opportunities for early intervention (JACR).
-
27% of Louisiana’s rural hospitals are vulnerable to closure, with 38% operating on negative margins (NRHA, 2024).
“Leakage" (patients going elsewhere for follow-ups) is the primary driver of lost outpatient revenue in rural-to-urban hospital networks (Pyatt et al, JACR 2020).
For every $1.00 spent on an incidental tracking system, the hospital realized $8.40 in new, net patient service revenue (Hardy et al, J Onc Practice 2021).
Hospitals implementing automated "closed-loop" tracking saw their follow-up completion rates jump from 21% to 64% in 18 months (AJR 2023).

The Solution

Advancing Rural Care with AI-Powered Radiology


AI-Driven Detection, Triage, and Follow-Up of Imaging Findings— Statewide Impact, Local Delivery
-
• Real-time analysis of CT/MRI/X-ray—detects anomalies with 92% sensitivity
• Automated triage: prioritizes high-risk cases for radiologist review
• Integrated follow-up: EHR-linked alerts, telehealth scheduling, patient portal reminders• Increased speed of MRI image acquisition using AI integration at the scanner
-
• Reduce patient travel by 70% (avg. 90-mile round-trip savings)
• Increase imaging finding follow-up completion from 35% to 85%• Improve hospital revenue via increased local imaging utilization
• Scalable: expandable to all 64 parishes by Year 2
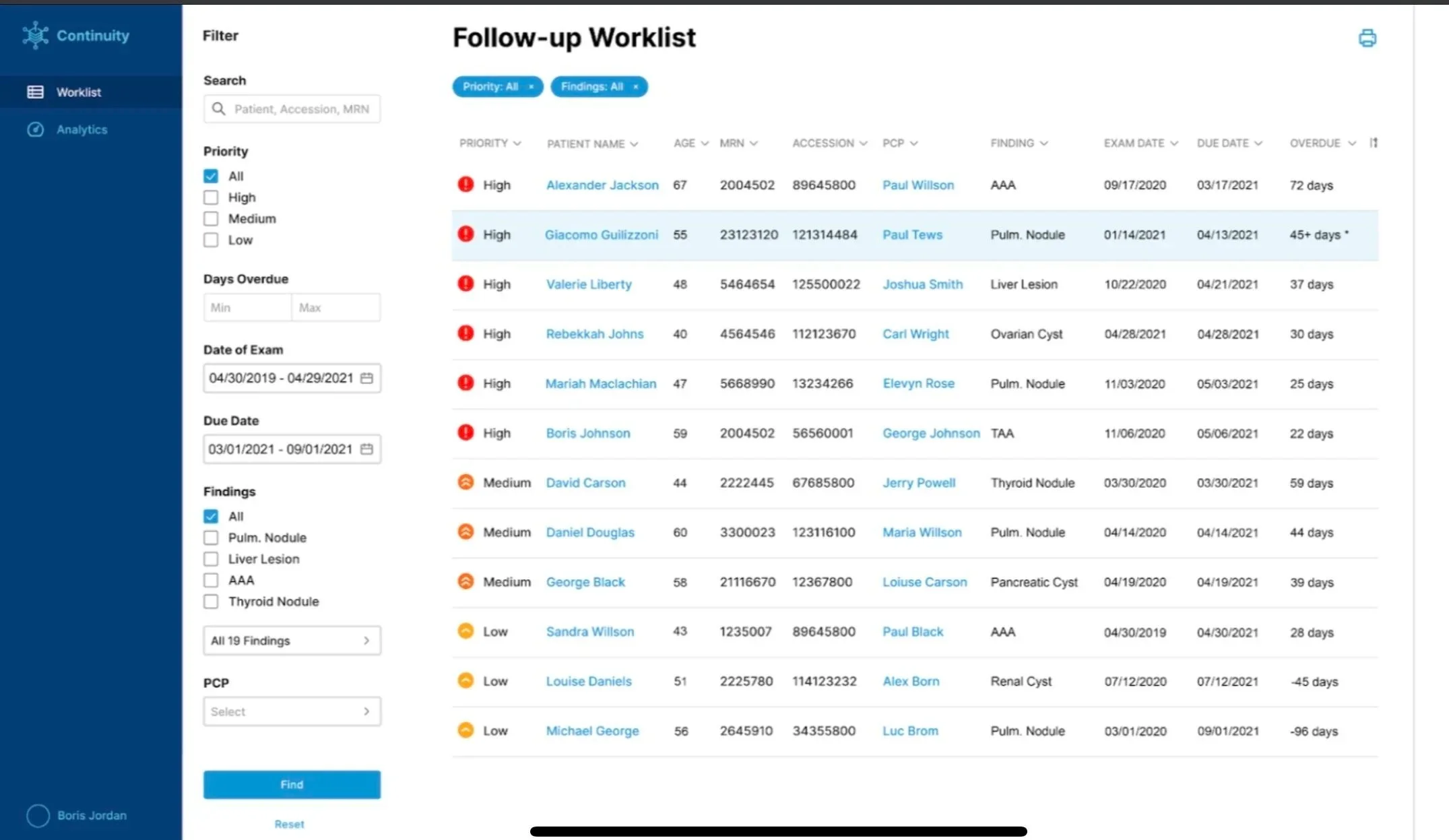
Figure 1 - Screenshot of Continuity AI software Dashboard interface with patient list and timeline data.
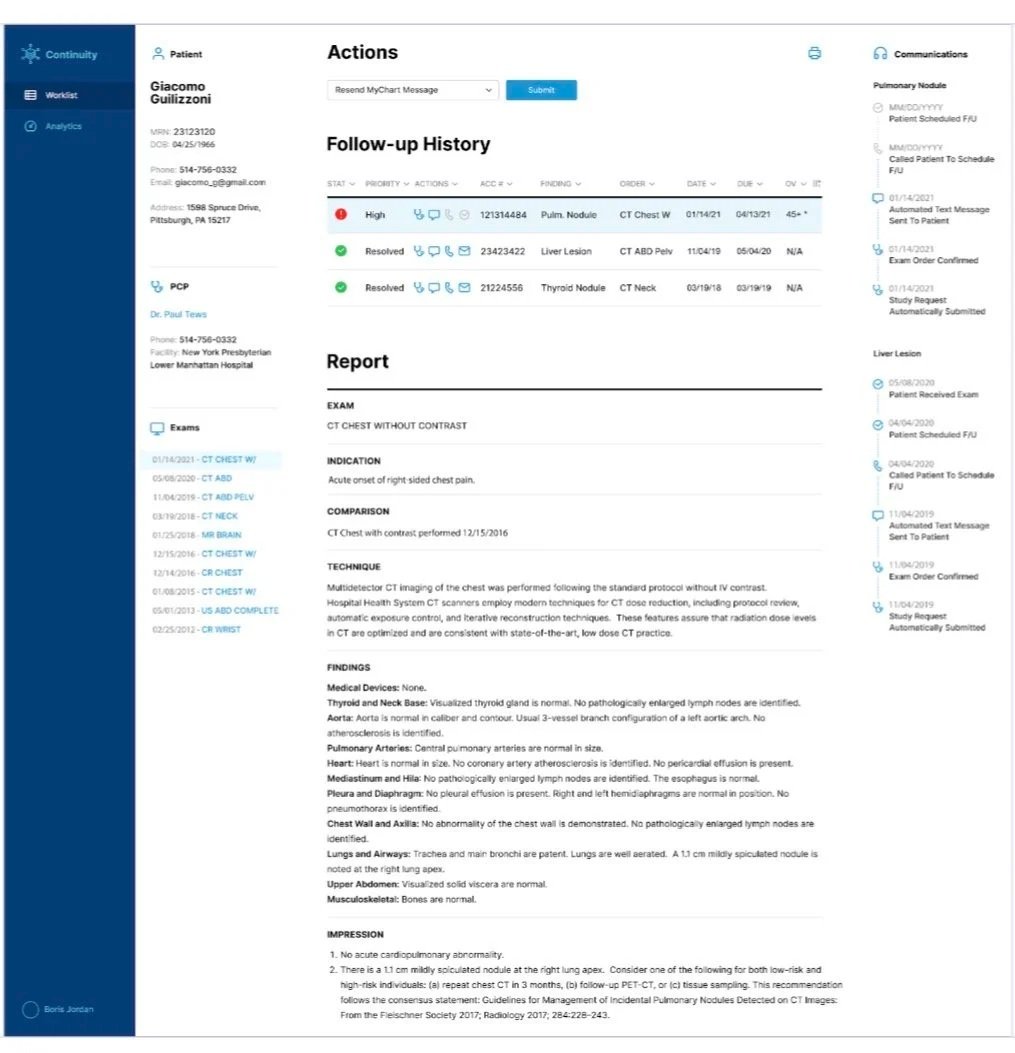
Figure 2 - Screenshot of Continuity AI software focus page demonstrating the task schedule for a single patient.

Figure 3 - Health System statistics demonstrating post-intervention and financial results.
Smart Detection
✳︎
Prioritized Alerts
✳︎
Local Oversight
✳︎
Seamless Follow-Up
✳︎
Data Security
✳︎
Smart Detection ✳︎ Prioritized Alerts ✳︎ Local Oversight ✳︎ Seamless Follow-Up ✳︎ Data Security ✳︎

The C.A.R.E. Pillars
-
We keep rural patients local. By automating follow-up scheduling, we ensure that specialized care is delivered within the patient’s own parish whenever possible.
-
We use enterprise-grade intelligence to triage and "look over the shoulder" of every clinician, flagging strokes and traumas in seconds to protect the 'Golden Hour.'
-
We solve the 'Outpatient Leakage' crisis. CARENET captures lost volumes and brings that technical fee revenue back to the rural hospital's bottom line.
-
We provide a 'Human-in-the-Loop' safety net. Our Navigators ensure that even our most vulnerable patients are never left behind in the diagnostic process including those without smartphones or reliable internet.

